Nursing Home Roommate Assignments, Cognitive Health, and Mortality
In 2025, nearly 1.2 million Americans lived in nursing homes. Medicaid and Medicare expenditures of $91 billion represented two-thirds of total revenues for nursing care facilities. With the prevalence of Alzheimer’s disease and Alzheimer's disease-related dementias (AD/ADRD) projected to rise as the US population ages, the need for nursing home care is expected to increase. Nearly 80 percent of nursing home patients are assigned shared rooms, which raises the question of whether having a roommate affects health outcomes.
In Patient Peer Effects: Evidence from Nursing Home Room Assignments (NBER Working Paper 34538), Alden Cheng and Martin B. Hackmann use data spanning 2000 to 2010 from the Centers for Medicare & Medicaid Services to examine 2.6 million patient stays across 7,200 nursing homes in 12 large states. These states account for approximately 60 percent of US nursing home patients. Patients’ room assignments are classified into three categories: rooms without roommates, rooms with at least one roommate with an AD/ADRD diagnosis, and rooms where none of the roommates have an AD/ADRD diagnosis.
Dementia patients experience lower mortality rates when assigned cognitively healthy roommates.
Potential benefits of shared rooms include companionship and cognitive stimulation for a population prone to loneliness. Potential downsides include sleep disruption, increased risk of infectious disease transmission, and exposure to behavioral disturbances—particularly among patients with AD/ADRD. Since only 4.5 percent of nursing home beds are in specialized dementia care units, which often feature single rooms, the majority of patients with AD/ADRD are in general care and may be assigned roommates.
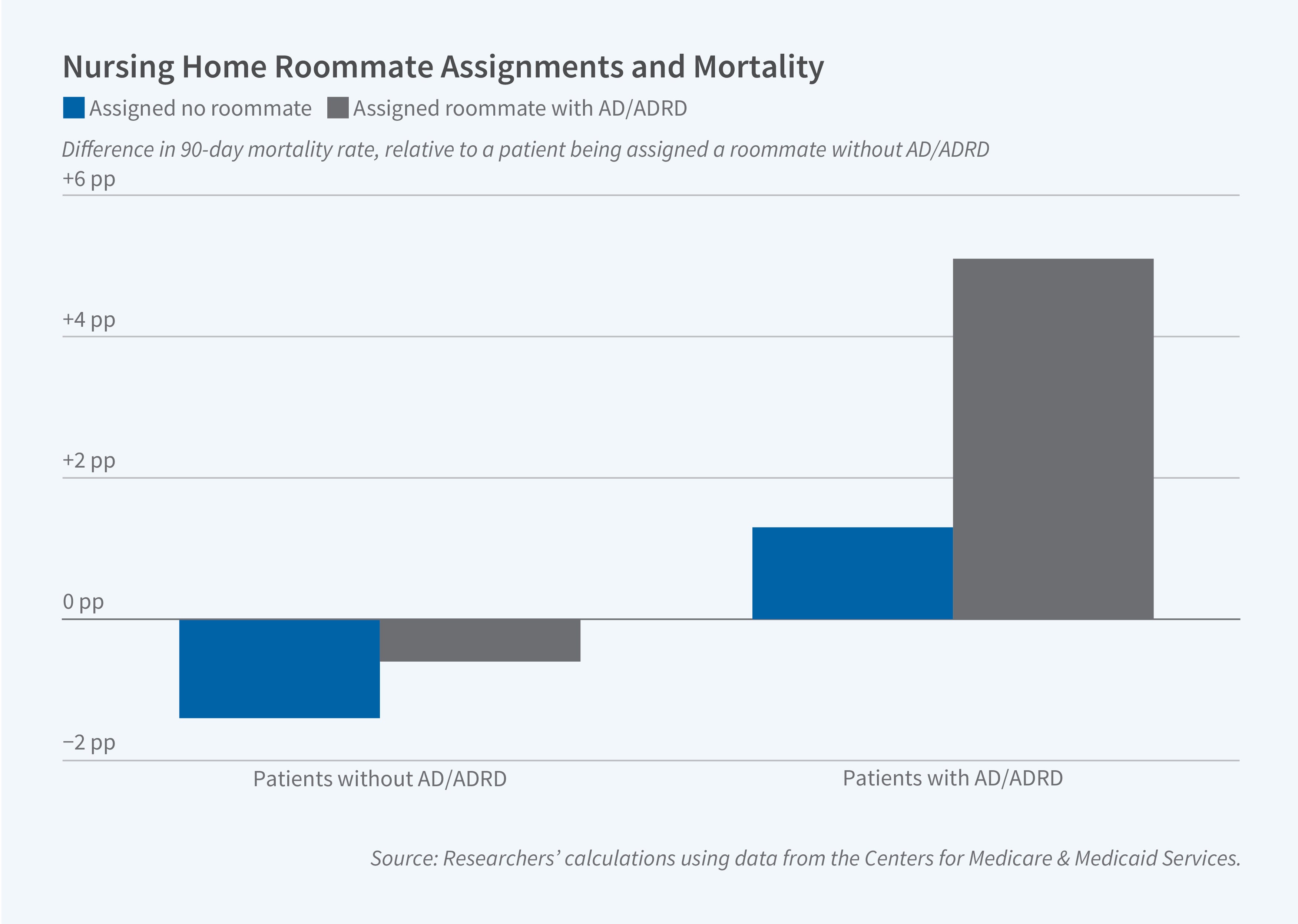
Using variation in room assignments that arises from bed availability at admission, the researchers find that, on average, being assigned no roommate reduces 90-day mortality by 1.3 percentage points relative to being assigned one—an 8.4 percent reduction relative to the mean. However, this mortality effect varies considerably with roommate characteristics. Relative to being assigned a cognitively healthy roommate, assignment to a private room reduces mortality by 0.7 percentage points, but being assigned a roommate with AD/ADRD increases mortality by 1.4 percentage points. Together, these estimates imply that moving from a private room to one shared with an AD/ADRD patient increases 90-day mortality by 2.1 percentage points.
The health impacts of room assignments depend on a patient’s own dementia status. Relative to having a cognitively healthy roommate, private room assignments reduce mortality for patients without dementia, but increase it for those with dementia. Having an AD/ADRD-diagnosed roommate increases mortality for patients with AD/ADRD by 5.1 percentage points while, for patients without AD/ADRD, the effect is statistically indistinguishable from zero.
Why do cognitively healthy roommates improve mortality rates of dementia patients? One possible explanation is that they provide informal monitoring, alerting staff when help is needed. Supporting this interpretation, the health benefits for patients with dementia are twice as large in facilities with below-median staffing levels and are concentrated among patients who are not in specialized Alzheimer's units.
The researchers suggest that strategic room assignment placing AD/ADRD patients with cognitively healthy roommates while prioritizing private rooms for patients without AD/ADRD could reduce 90-day mortality rates by 0.8 percentage points (5.2 percent) without requiring additional staffing or facility modifications.
- Leonardo Vasquez
The researchers acknowledge support from National Institute on Aging grant #P01 AG005842-29.


