How Patients Fare When Private Equity Funds Acquire Nursing Homes
Purchases of nursing homes by private equity firms are associated with higher patient mortality rates, fewer caregivers, higher management fees, and a decline in patient mobility.
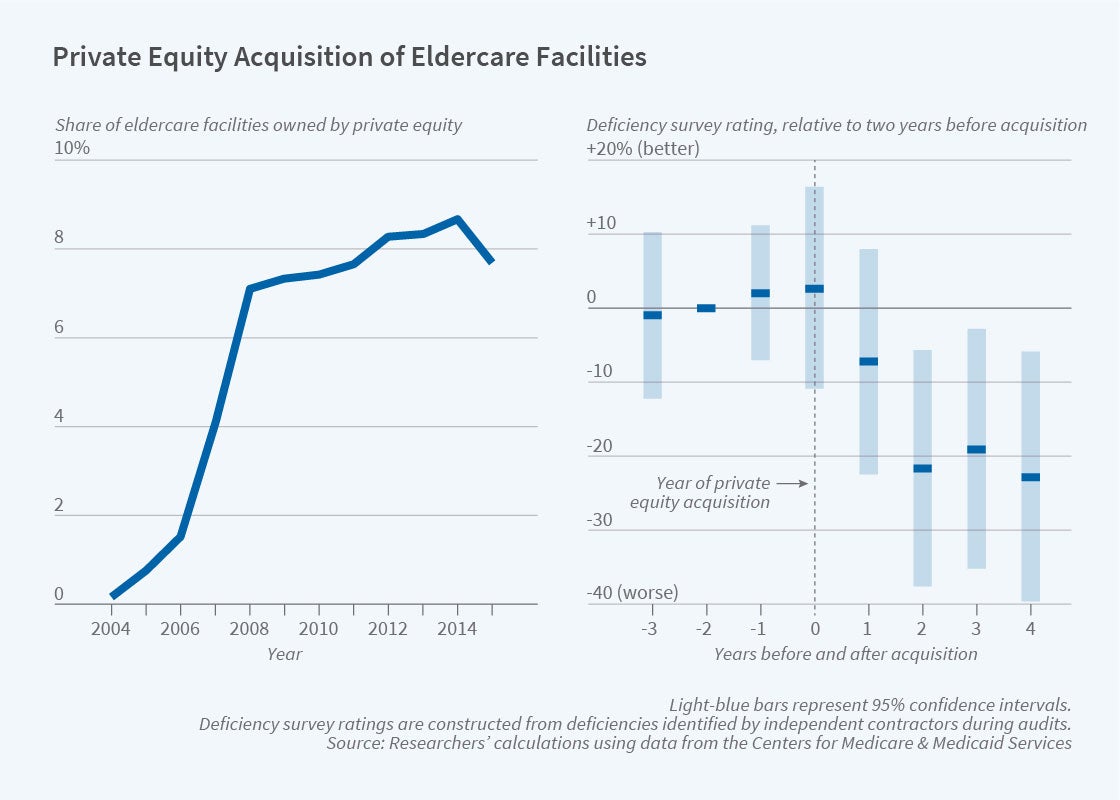
In 2005, private equity-owned firms owned less than 1 percent of skilled nursing facilities. By 2015, they owned 9 percent; the share is likely higher today. A new study explores the impact of their business model on patient outcomes and costs. In Does Private Equity Investment in Healthcare Benefit Patients? Evidence from Nursing Homes (NBER Working Paper 28474), Atul Gupta, Sabrina T. Howell, Constantine Yannelis, and Abhinav Gupta analyze Medicare data for a sample of more than 7 million patients over the period 2005–2017. They find that the patient mortality rate during a nursing home stay and the subsequent 90 days is 10 percent higher at facilities owned by private equity firms than at skilled nursing facilities overall.
Private equity-owned nursing homes face vastly different financial considerations than their for-profit and not-for-profit competitors. Private equity buyouts are typically financed with substantial borrowing. Analysis of the cost reports submitted to Medicare shows that after a buyout, a nursing home’s average interest payments more than triple. To generate cash for investors, private equity managers often sell the nursing facility’s property and lease the building back; this results in an average increase in lease payments of 75 percent post-buyout. Cash on hand declines by 38 percent after a private equity acquisition. This may leave homes hard-pressed to respond to something like a sudden need for personal protective equipment during the COVID-19 pandemic.
To cut costs, private equity-owned nursing homes reduce staffing levels. Frontline caregivers — clinical nursing assistants and licensed practical nurses — see a 3 percent decline in hours compared with the industry average. However, registered nurses, who make up a much smaller segment of the care staff, see an 8 percent increase. The researchers attribute this increase to greater regulatory focus on registered nurses; for example, their availability is a factor in determination of Medicare reimbursements.
Taking the results on nurse availability together with the estimated effects on interest, lease, and management fees payments, the researchers infer that private equity ownership shifts operating costs away from staffing towards costs that are profit drivers for the private equity fund.
Private equity ownership on average leads to higher charges. The overall bill is more than 10 percent higher if a patient goes to a private equity-owned nursing home than another home.
The higher fees do not translate into better care, as measured by key Medicare indicators. Patients admitted to private equity-owned nursing homes are 50 percent more likely to be placed on antipsychotic medication. By sedating patients rather than applying behavioral therapy, nursing homes can reduce staffing needs. Private equity-owned homes also perform below average in two other key metrics of well-being: patients experience a greater decline in mobility and increased levels of pain.
— Steve Maas


