Hospital C-Section Rates and Infant Health
Rates of cesarean delivery in the United States — approximately one-third of all births — are substantially higher than in many other developed nations. In addition, risk-adjusted cesarean delivery rates vary considerably across hospitals, raising important questions about why they differ and how these differences in practice style may affect patients. In The Health Impacts of Hospital Delivery Practices (NBER working paper 25986), researchers David Card, Alessandra Fenizia, and David Silver examine the impact of delivering a baby at a hospital that has a relatively high C-section rate.
These findings suggest both benefits and costs from the earlier truncation of long labors that occurs at high c-section hospitals.
The researchers focus on low-risk first births — which constitute about 15 percent of all births — between 2007 and 2011, using data from California’s Office of Statewide Health Planning and Development. They classify hospitals as having a “high” C-section rate if the risk-adjusted rate is higher than the average within their hospital referral region. Using this classification and sample, the average C-section rate is 29 percent in hospitals that are designated as having high C-section rates and 22 percent at other hospitals.
While there are many factors that may affect a patient’s choice of hospital, mothers tend to deliver at the nearest hospital. In fact, for every 10 miles closer that a mother lives to a high C-section hospital, the researchers estimate that she is 15.9 percentage points more likely to deliver at such a hospital. Furthermore, she is 1.86 percentage points more likely to deliver via c-section. Most of this increase in the likelihood of cesarean delivery is offset by a decline in vaginal births after prolonged labors.
In order to estimate the health effects of a hospital’s practice style, the researchers rely solely on the variation in hospital choice that arises from the relative distance to different types of hospitals. This approach allows them to separate the impact of hospital practice style from the impact of other factors that might also contribute to hospital choice, such as health status or insurance status.
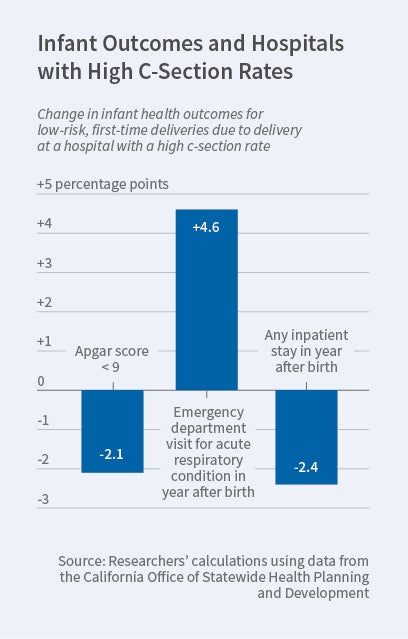
The existing literature suggests that babies delivered by C-section are at elevated risk of breathing problems. Consistent with this view, the researchers find that newborns delivered at a high C-section hospital are more likely to receive ventilation assistance immediately after delivery and are at greater risk of visiting the emergency department during their first year, mostly for acute respiratory conditions.
However, as shown in the figure, delivery at high C-section hospitals improves other infant health outcomes. For example, 5-minute Apgar scores, which are indicators of newborn health, are better. In addition, infants born in these hospitals are 2.4 percentage points less likely to have an inpatient stay during their first year. There is also some evidence that infant mortality is lower for infants born in these hospitals.
Taken together, these findings suggest both benefits and costs from the earlier truncation of long labors that occurs at high C-section hospitals. The documented benefits run counter to claims that the US necessarily has an excessive C-section rate and, in particular, that hospitals with intensive practice styles are necessarily delivering worse care.
— Robin McKnight
Silver acknowledges funding from the National Institute on Aging, Grant Number T32-AG000186.