Costs and Consequences of COVID’s Impact on Nonurgent Care
A new study of COVID-19-related disruptions in health care sheds light on the value of nonurgent medical care. In Mortality Effects of Healthcare Supply Shocks: Evidence Using Linked Deaths and Electronic Health Records (NBER Working Paper 30553), Engy Ziedan, Kosali I. Simon, and Coady Wing compare people who had outpatient appointments scheduled in the 30 days immediately before the March 13, 2020, pandemic declaration with those who had appointments scheduled in the 30 days afterward.
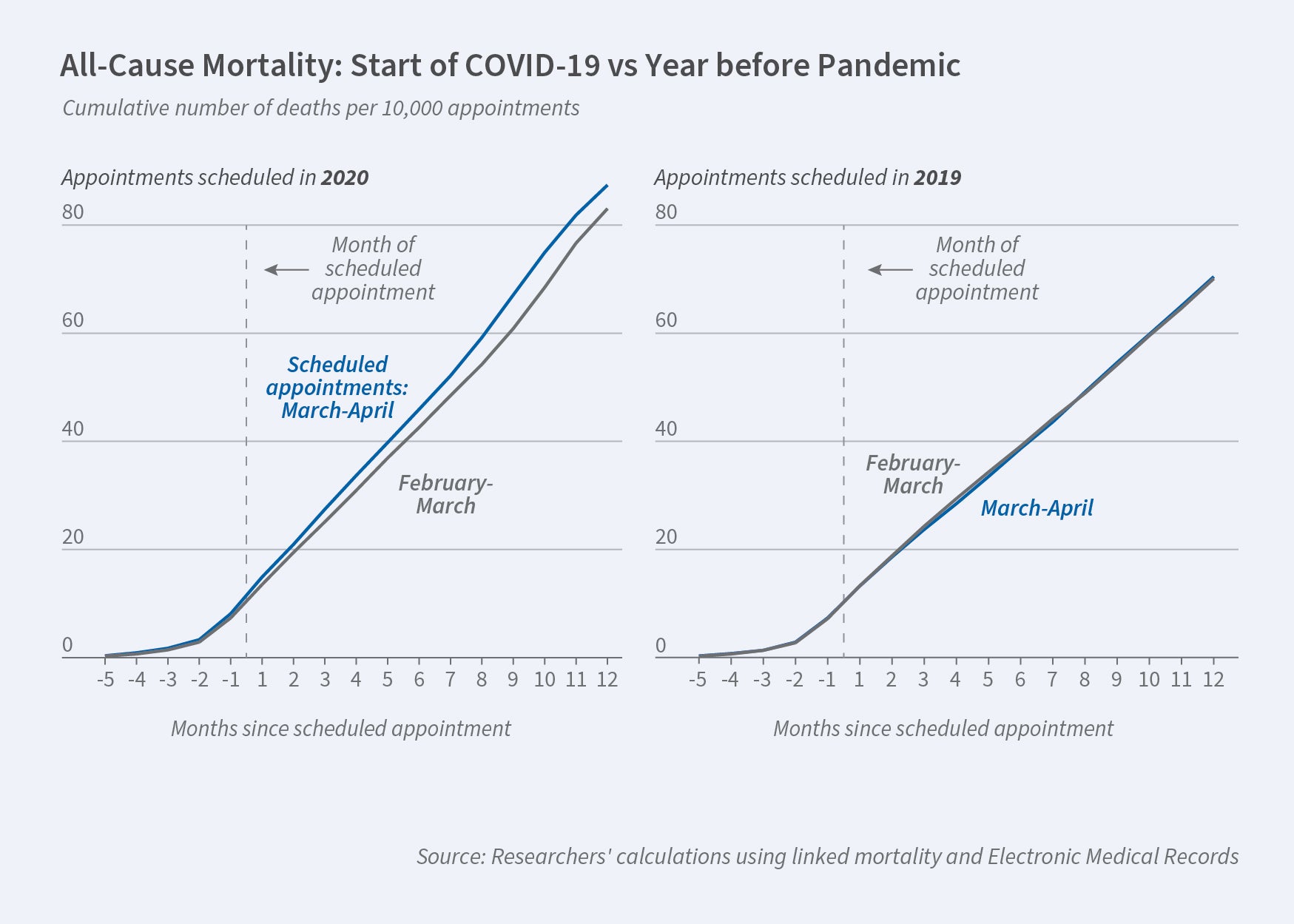
They find that the appointment cancellation rate post-declaration was nearly 34 percent compared with 19 percent in the month before declaration. The figure shows that in 2020, the one-year mortality rate for the post-declaration group was 87 deaths per 10,000 appointments over the course of the next year, compared with 83 deaths for the pre-declaration group. This implies roughly one additional death for every 333 canceled appointments. Such differences were not observed for similar adjacent cohorts in 2019 (right panel in figure).
Every 333 canceled outpatient appointments in the 30 days after the pandemic led to one life lost in the following year.
The study draws on data from more than 3.1 million scheduled appointments in the 30 days before the pandemic declaration, and more than 2.5 million afterward. Those who were induced to cancel appointments because of the timing of the pandemic emergency tended to be sicker and older than the overall study population, suggesting that they may have stayed home out of fear of COVID-19. Individuals in the group with post-declaration appointments also accumulated fewer additional appointments in the three months after their initial scheduled visit than their counterparts in the pre-declaration appointment group, which compounded the effects on health outcomes. This suggests the absence of follow-up sessions that might have resulted in health benefits.
While appointment data do not include details on tests and procedures, they do specify types of providers. Among the post-declaration group, 64 percent of those who canceled appointments were scheduled to see a specialist compared with 56 percent of the earlier group.
Canceled appointments increased mortality rates by more than twice as much for those over 65 as for those under 65. For those with two or more comorbidities, the increase in the mortality rate was five times greater than for those with one or two comorbidities. Overall, the researchers estimate that cancellations explain between a quarter and a third of non-COVID excess deaths between March 2020 and March 2021.
To translate the elevated mortality rates of those who canceled appointments into economic terms, the researchers assume that all deaths before age 75 are premature, from which it follows that for every 10,000 canceled appointments, 443.5 life years were lost. If a lost statistical life year is worth $150,000, the monetary value of an outpatient visit is at least $3,000, more than 10 times the average appointment cost of $300.
The researchers acknowledge support from the National Institutes of Health under contract # 75N95D20F4000.
—Steve Maas


