Market Failure in Kidney Exchange
For individuals with chronic kidney disease, a kidney transplant is a life-saving medical intervention, often preferable to dialysis in terms of the expected length and quality of life. Currently, nearly 100,000 patients are on the wait list for a kidney from a deceased donor and the average wait time is years long. While some patients have a family member or friend willing to donate a kidney to them, the donor and recipient must be compatible in blood and tissue type in order for a direct donation to be feasible.
The kidney exchange market in the U.S. enables transplants each year for about 800 patients with a willing live but incompatible donor. In Market Failure in Kidney Exchange (NBER Working Paper No. 24775), researchers Nikhil Agarwal, Itai Ashlagi, Eduardo Azevedo, Clayton Featherstone, and Ömer Karaduman explore the workings of the kidney exchange market.
Kidney exchanges are organized when two or more incompatible donor-recipient pairs are swapped to create compatible matches, or when an altruistic (unpaired) donor provides a kidney and this enables a chain of compatible pairs to be formed. Kidney exchanges are organized through three large national platforms as well as within hospitals. There are some incentives for hospitals to use these platforms, such as receiving an organ for an unpaired patient if they provide an altruistic donor. The platforms use optimization software to maximize the number of matches (weighted to give priority to some patients, such as previous live donors and hard to match patients). Due to biological compatibility, some matches are inefficient. For example, a patient with blood type O can only receive a donation from an O donor, while a patient with blood type A can receive a donation from an A or an O donor. Matching an O donor with an A recipient is inefficient because it makes it more likely that there will be an unmatched O patient.
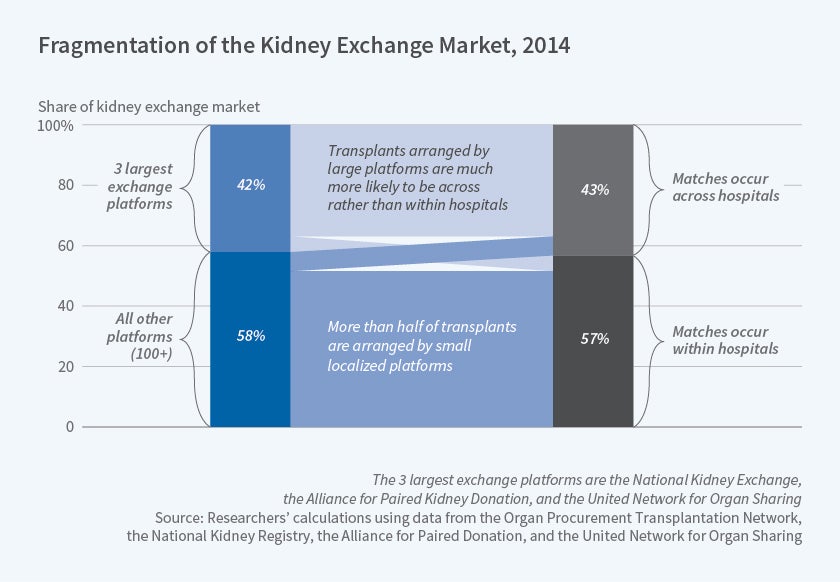
The researchers first document the fragmentation in the kidney exchange market. In 2014, the three largest platforms arranged only 42 percent of the exchanges, while hospitals or small regional platforms arranged 58 percent. Furthermore, hospitals or small regional platforms nearly always arrange transplants within hospitals (with a donor and recipient from the same hospital), whereas the national platforms nearly always arrange transplants across hospitals. This is potentially important because national platforms can take advantage of their larger donor and recipient pools to arrange for more efficient matches.
Indeed, the case of O donors and recipients provides evidence of this. In transplants arranged by the national platforms, only 7 percent of O donor organs are used for non-O patients, while this rate is 23 percent for transplants organized by hospitals and small platforms. More generally, in the transplants they arrange, hospitals often transplant kidneys from easy-to-match donors to easy-to-match recipients, which will tend to leave harder-to-match recipients unmatched. Hospitals also seem to be sensitive to the financial and administrative costs of participating in a large exchange and typically do not conduct all of their exchanges through a national platform even if they use it sometimes.
The researchers develop a theoretical model to explain these facts. Their analysis suggests that hospitals would be more likely to participate in a national platform if they were awarded points in accordance with the value of the additional matches made possible by their donations. The analysis also suggests that subsidies could offset the costs that discourage hospitals from participating in national platforms.
Finally, the researchers project that addressing the fragmentation in the U.S. kidney exchange market could generate an additional 200 to 440 additional transplants per year, representing a 25 to 55 percent increase over the current number of live donor transplants.
In concluding, the researchers note that there are some pilot programs under way that would award points for organ donations and cover the costs of participating in the national platforms. Overall, "[o]ur results indicate that there could be large gains from continuing to move in this direction."
The authors acknowledge funding from Wharton's Dean's research fund and the National Science Foundation (SES-1254768).