Understanding Changes in Healthy Life Spans
Although it has long been known that life expectancy at older ages is increasing, it is less clear whether people are living healthier as well as longer lives. While researchers who focus on disease prevalence find that people are spending more years living with disease, those who focus on disability reach the opposite conclusion. Even less is known about why these changes in healthy life span are occurring.
In Understanding the Improvement in Disability-Free Life Expectancy in the U.S. Elderly Population (NBER Working Paper No. 22306), researchers Michael Chernew, David Cutler, Kaushik Ghosh, and Mary Beth Landrum take up these issues.
The authors use disability as their measure of health. One reason to focus on disability rather than disease is that some chronic diseases can be effectively managed with medication or lifestyle changes; indeed, research suggests that disability conditional on disease has declined over time. Disability is defined here as having difficulty with any Activity of Daily Living or Instrumental Activity of Daily Living, which include functions such as walking and bathing (ADLs) and doing housework and managing money (IADLs).
The authors' first goal is to estimate changes over time in disabled and non-disabled life expectancy, which is the number of years a 65-year-old person can expect to live with and without any disability. To do so, the authors use data from Medicare Current Beneficiary Survey (MCBS) for two periods, 1991-94 and 2006-09. For each period, they estimate models that relate disability to age, sex, and time until death. They then use the results to predict the probability of disability for each individual and average these predictions by single year of age. Finally, they match these age-specific disability rates to life tables in 1992 and 2008 to estimate years of disabled and non-disabled life expectancy.
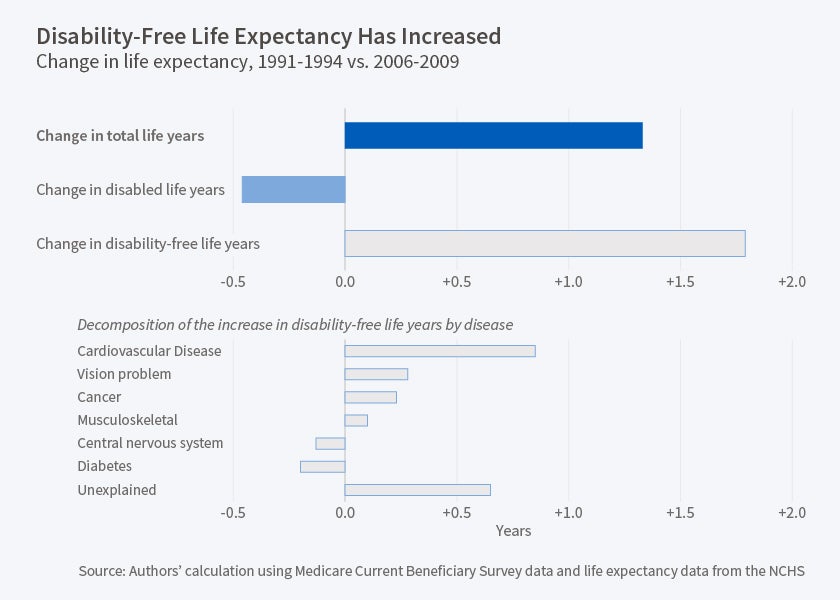
In 1992, total life expectancy at age 65 was 17.5 years. This was divided nearly evenly into an expected 8.9 years without disability and 8.6 years with disability. By 2008, total life expectancy had increased by 1.3 years, to 18.8 years. But disability-free life years increased by even more, 1.8 years, while disabled life years shrank by 0.5 years. Thus, whether one focuses on the number of years or on the share of remaining life expectancy, disability is being compressed into the period just before death.
A second key goal is to estimate the contribution of various diseases to the change in disabled and non-disabled life expectancy. Here the authors first estimate models for each period relating disability to the presence of various diseases, demographic characteristics, and time until death. The authors then replace the actual incidence of each disease and the estimated relationship between that disease and disability that existed in the earlier period with those from the later period and calculate the impact of this switch on life expectancy.
Changes in cardiovascular disease are responsible for nearly half of the overall increase in disability-free life expectancy over this 15-year period—0.85 of the 1.8 years. Reductions in the incidence of vision problems and in the probability of disability among cancer survivors are responsible for further increases of 0.28 and 0.23 years of disability-free life expectancy, respectively. By contrast, increases in the prevalence of diabetes and in both the incidence and disabling impact of central nervous system diseases such as Alzheimers and Parkinsons have reduced disability-free life expectancy.
A final central question is how much of the rise in disability-free life expectancy can be explained by increases in the use and efficacy of medical treatments. The authors focus on cardiovascular disease and vision problems, the two conditions that contributed the most to the overall increase. It is particularly challenging to estimate the impact of treatment on outcomes because treatment is non-random, with those patients who are sicker being more likely to receive medical care. To surmount this difficulty for cardiovascular disease, the authors use a well-established model that estimates the contribution of treatments and risk factors to mortality, along with data on changes in the use of medical treatment and risk factors over time. For vision problems, the authors estimate models relating disability to the use of cataract surgery.
Describing these results as more speculative, the authors conclude that roughly half of the mortality reduction from cardiovascular disease results from improved medical treatments, which translates into about 0.26 years, or 15 percent, of the overall increase in disability-free life expectancy. For vision problems, they estimate that one-quarter of the reduction in disability due to vision problems is due to greater use of cataract surgery, which equates to about 0.08 years, or 5 percent, of the increase in non-disabled life.
The authors note that one limitation of their study is that their data do not allow them to explore the role of mental health and musculoskeletal issues, which have been shown to be important contributors to disability. Recent work has also highlighted a slowdown or reversal in health gains among the near elderly as well as the concentration of health gains among those with high socioeconomic status. Further work exploring all of these issues would greatly inform our understanding of how healthy life spans are evolving for the elderly.
The authors acknowledge funding from the National Institute on Aging (P01 AG005842) and Pfizer. At least one coauthor has disclosed a financial relationship of potential relevance for this research. Further information is available at http://www.nber.org/papers/w22306.ack