Measuring the Virus Risk of Essential Workers and Dependents
Data on 800,000 commercially insured individuals in Philadelphia suggest that during lockdown essential workers were 55 percent more likely than others to get COVID-19.
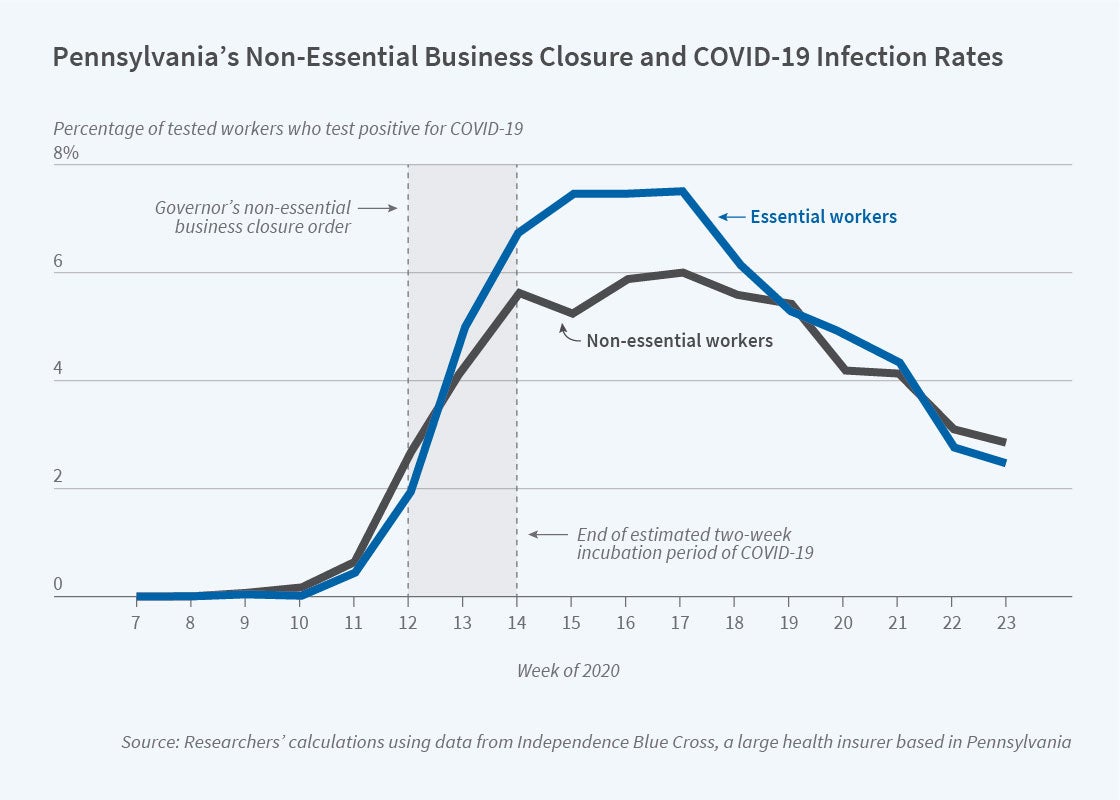
For 12 weeks beginning in March 2020, Pennsylvania closed all nonessential businesses as part of a program to reduce the spread of COVID-19. A new study examines how this lockdown affected the relative health of employees in essential and nonessential businesses.
In The Impact of the Nonessential Business Closure Policy on COVID-19 Infection Rates (NBER Working Paper 28374), Hummy Song, Ryan M. McKenna, Angela T. Chen, Guy David, and Aaron Smith-McLallen analyze medical claims data from Independence Blue Cross, which covers more than half of the commercially insured individuals in Greater Philadelphia. They combine this with zip-code-level demographic and economic data to control for factors that could affect COVID-19 illness rates, such as age, gender, occupation, socioeconomic status, comorbidities, and virus time trends.
The data sample consists of 416,000 primary policyholders and 387,000 cohabiting dependents covered by the primary policyholder. The average coronavirus positivity rate of people in the sample is 1.36 percent.
The researchers find that the share of essential workers who receive a positive test result is 0.76 percent higher than the share of non-essential workers, a gap of 55 percent relative to the population average. Even after excluding those in the health care and social assistance sectors, who are more likely to have intimate, prolonged contact with infected patients, the remaining essential workers are 21 percent more likely to become infected than nonessential workers. They also find that dependents living with essential workers face a risk of infection 17 percent higher than those living with nonessential workers, and that nondependent, nonessential workers who live with essential workers — mostly adult roommates — have a 38 percent higher probability of testing positive.
The researchers caution that since their sample includes only commercially insured individuals, the results may not be fully applicable to the general population. Their findings may in fact underestimate the risks faced by households of the many essential workers who have no insurance coverage, such as part-time grocery clerks, home health aides, and independent delivery drivers.
The researchers note that while in normal times workers take on high-risk jobs in return for higher pay or job satisfaction, during the pandemic the risks for essential workers have increased with little or no change in compensation. They argue that the disproportionate health risks faced by essential workers and their families should be recognized when policymakers weigh the costs and benefits of expanding economic activity amid a pandemic.
— Steve Maas